How to Get Rid of a Headache Fast: Proven Relief Methods That Work
That throbbing pain just started — and you need relief now. To get rid of a headache fast, immediately drink a glass of water, apply a cold compress to your forehead or neck, and rest in a quiet, dark room. These three steps alone can ease pain within minutes. For tension headaches, gently massage your temples and neck, take a hot shower, or try light neck stretches.
Headaches can strike at any time, disrupting your focus, mood, and daily routine. Whether yours is caused by stress, dehydration, poor posture, or lack of sleep, fast relief is possible. In this guide, you’ll find simple, science-backed remedies — ranked from fastest to slowest — so you can choose what works best for your situation. In this guide, you’ll discover practical and quick solutions to get rid of a headache fast and feel better naturally.
Common Causes of Headaches

Headaches can happen for many different reasons, often linked to daily habits and lifestyle factors. Understanding the root cause can help you prevent them and find faster relief. Here are a few common causes:
Dehydration
Even mild dehydration (losing just 1–2% of body fluid) can reduce blood flow to the brain and trigger a headache. Drinking 1–2 glasses of water at the first sign of pain is often enough to get relief.
Stress and Anxiety
High stress levels and anxiety can tighten muscles in your head, neck, and shoulders, leading to tension headaches that feel like constant pressure.
Lack of Sleep
Poor or insufficient sleep disrupts your body’s balance and can make you more sensitive to pain, increasing the chances of headaches.
Poor Diet or Skipping Meals
Poor Diet or Skipping Meals — Drops in blood sugar (hypoglycemia) from skipping meals trigger what are sometimes called “hunger headaches.” Eating small, regular meals with complex carbohydrates helps stabilize blood sugar and prevent these episodes.
Screen Time and Digital Eye Strain
Prolonged screen use causes a condition called Computer Vision Syndrome (CVS), which leads to eye strain, blurred vision, and headaches. The 20-20-20 rule (look 20 feet away for 20 seconds every 20 minutes) is an effective preventive measure.
Hormonal Changes
Hormonal fluctuations, especially in women, can trigger headaches. Changes during menstruation, pregnancy, or menopause are common causes.
Types of Headaches Explained
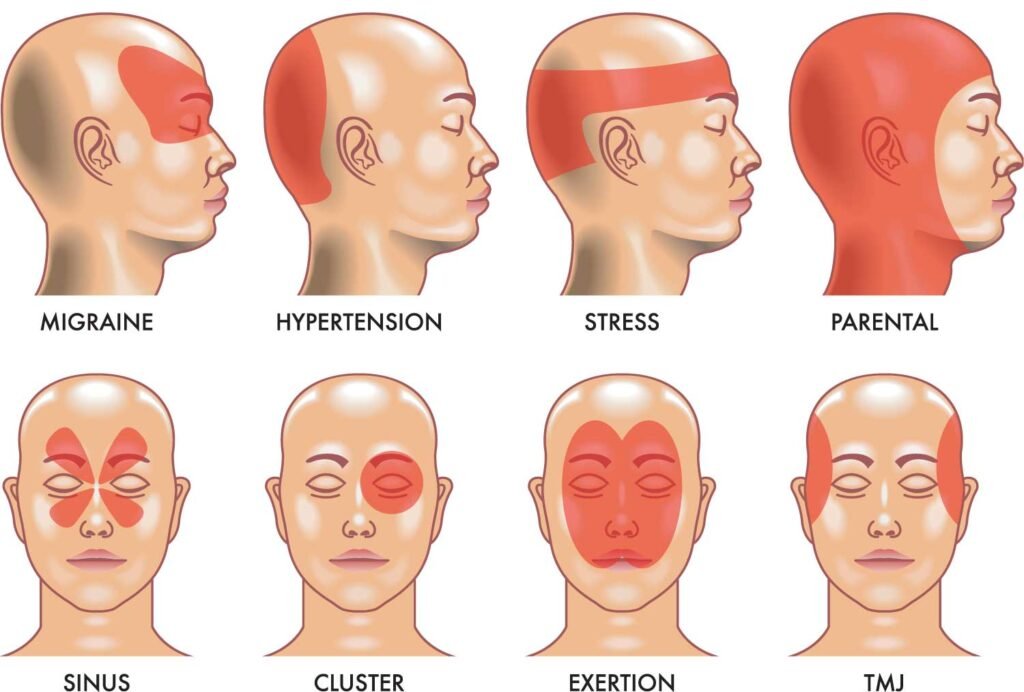
Headaches can feel different depending on their cause, and knowing the type can help you choose the right treatment. Here are the most common types explained in a simple way:
Tension Headache — The most common headache type, affecting up to 78% of the general population at some point. It feels like a constant, dull pressure — like a tight band squeezing your forehead or the back of your head. Stress, poor posture, and prolonged screen use are the most frequent triggers. Best relieved with: warm compress, neck massage, ibuprofen.
Migraine — A neurological condition affecting about 1 in 7 people worldwide. The pain is intense, throbbing, and typically one-sided, often accompanied by nausea, light/sound sensitivity, and in some cases, visual disturbances called “aura.” Migraines can last 4–72 hours. Best relieved with: cold compress, dark room, prescribed triptans, or OTC ibuprofen at onset.
Sinus Headache — Sinus headaches are linked to sinus infections or congestion. They cause pressure and pain around your forehead, cheeks, and eyes. The pain often gets worse when you bend forward or move your head. You may also have a runny or blocked nose along with the headache.
Cluster Headache — Among the most painful conditions known to medicine, cluster headaches occur in cyclical patterns — typically 1–3 attacks per day for several weeks, followed by remission periods. Pain is sharp, burning, and concentrated around one eye. If you suspect cluster headaches, consult a neurologist — they require prescription treatment.
Instant Ways to Get Rid of Headache
When a headache hits, you want quick relief. These simple and effective methods can help reduce pain fast without complicated treatments:
Apply a Cold Compress (Best for migraines) — Wrap ice in a cloth or use a cold gel pack and apply it to your forehead or the back of your neck for 10–15 minutes. Cold constricts blood vessels, which reduces the throbbing sensation associated with migraines. Do not apply ice directly to skin.
Use a Warm Compress (Best for tension headaches) — Apply a warm towel or heating pad to the back of your neck or shoulders for 15–20 minutes. Heat increases blood flow and relaxes the tight muscles that cause tension-type pain. This is especially effective when combined with gentle neck stretches.
Drink Water — Dehydration is one of the most common causes of headaches. Drinking a glass or two of water can sometimes relieve pain within minutes. Make it a habit to stay hydrated throughout the day to prevent recurring headaches.
Take Rest in a Dark Room — Bright lights and noise can worsen headaches, especially migraines. Lying down in a quiet, dark room allows your brain to relax and reduces sensory triggers, helping the headache fade more quickly.
Try a Small Amount of Caffeine — One cup of coffee or tea can help narrow dilated blood vessels and boost the effectiveness of pain relievers like acetaminophen by up to 40% (this is why caffeine is an active ingredient in Excedrin). Limit to one cup. Important: If you consume caffeine daily and suddenly stop, withdrawal itself can cause a headache.
Massage Your Head and Neck — Gently massaging your temples, scalp, neck, and shoulders can improve blood circulation and relieve muscle tension. This is particularly helpful for stress-related headaches and can provide quick comfort.
Try Diaphragmatic Breathing (4-7-8 Technique) — Stress and shallow breathing reduce oxygen flow and can intensify headache pain. Practice the 4-7-8 method: inhale for 4 seconds, hold for 7, exhale for 8. Repeat 4 cycles. This activates the parasympathetic nervous system, reducing tension and stress hormones that worsen pain.
Natural Remedies for Headache Relief

If you prefer a natural approach, there are several simple remedies that can help reduce headache pain without relying on medication. These methods are safe, effective, and easy to include in your daily routine:
Ginger Tea
Research published in Phytotherapy Research found that ginger powder was as effective as sumatriptan (a common migraine drug) in reducing migraine severity. Steep 1 teaspoon of fresh grated ginger in hot water for 5 minutes. Drink at the first sign of a headache for best results. Also helps with migraine-associated nausea.
Peppermint Oil
A study in Cephalalgia journal found that topical 10% peppermint oil (menthol) applied to the forehead and temples significantly reduced headache intensity within 15 minutes. Always dilute with a carrier oil (like coconut oil) before skin application. Avoid contact with eyes.
Lavender Oil
Lavender oil is known for its calming and stress-relieving properties. Inhaling its aroma or applying diluted oil to your temples can reduce headache intensity, especially those caused by stress or anxiety. It also promotes relaxation and better sleep.
Magnesium-Rich Foods
Low magnesium levels are linked to headaches, particularly migraines. Eating foods rich in magnesium—like leafy greens, nuts, seeds, and whole grains—can help prevent headaches and support overall brain health.
Proper Sleep Routine
Both too little AND too much sleep can trigger headaches. Aim for 7–9 hours per night (adults) with consistent bed/wake times, even on weekends. Avoid screens 30 minutes before bed — blue light suppresses melatonin and disrupts sleep quality, increasing headache risk the next day.
Best Medicines for Headache Relief

Medications can provide fast and effective relief from headaches, especially when home remedies aren’t enough. The right choice depends on the type and severity of your headache:
Over-the-Counter Options
For mild to moderate headaches, over-the-counter (OTC) medicines are often the first choice. Ibuprofen (Advil, Motrin) — 200–400 mg at onset. Effective for both tension headaches and migraines. Take with food to reduce stomach irritation.
Not recommended if you have kidney issues or are on blood thinners. Acetaminophen (Tylenol) — 500–1000 mg. Gentler on the stomach; preferred for those who cannot take NSAIDs. Do not exceed 3,000 mg/day. Aspirin — 500–650 mg. Effective but not suitable for children under 16, pregnant women, or those with stomach ulcers.
Prescription Treatments
For severe or frequent migraines (3+ per month), doctors may prescribe triptans (such as sumatriptan or rizatriptan), CGRP inhibitors (a newer class), or preventive medications like beta-blockers or topiramate. These must be used under medical supervision. Never self-medicate with leftover prescription drugs.
Important: Taking any headache medication more than 10–15 days per month can lead to medication overuse headache (MOH), also called rebound headache. so it’s best to consult a healthcare professional for proper guidance.
When to See a Doctor?
While most headaches are harmless, some can signal a more serious issue. It’s important to seek medical attention if you notice any of the following warning signs:
- Thunderclap headache (worst headache of your life): A sudden, severe headache reaching peak intensity within 60 seconds can indicate a subarachnoid hemorrhage (brain bleed) — a medical emergency. Call emergency services (911) immediately. Do not wait to “see if it gets better.
- After a head injury: Headaches following a fall, accident, or injury should not be ignored, especially if they worsen over time.
- Vision or speech problems: Blurred vision, double vision, difficulty speaking, or confusion along with a headache may point to a neurological issue.
- Headaches occurring more than 15 days per month (Chronic Daily Headache): This frequency requires medical evaluation. Your doctor can rule out underlying causes and discuss preventive treatment options. Tracking your headaches in a diary before the appointment significantly helps diagnose and get proper treatment.
Tips to Avoid Future Headaches

Preventing headaches is often easier than treating them. Small lifestyle changes can make a big difference in reducing how often headaches occur:
Keep a Headache Diary
date/time, duration, pain level (1–10), location on head, possible triggers (food, stress, sleep, weather), and any medications taken. Apps like Migraine Buddy or N1-Headache make this easy. Sharing 4+ weeks of diary data with your doctor dramatically improves the accuracy of diagnosis. This helps you identify personal triggers such as certain foods, weather changes, or daily habits. Over time, you can adjust your routine to avoid those specific triggers.
Reduce Screen Time
Spending too much time on screens can strain your eyes and overstimulate your brain. Try following the 20-20-20 rule—every 20 minutes, look at something 20 feet away for 20 seconds. This simple habit can reduce digital fatigue and lower your chances of developing headaches.
Improve Posture
Poor posture, especially while sitting or working, can put extra pressure on your neck and shoulders. Keeping your back straight and your screen at eye level helps reduce strain on muscles. Good posture supports better blood flow and prevents tension buildup that can lead to headaches.
Eat Balanced Meals
Aged cheeses, processed meats (containing nitrates), red wine, MSG, and artificial sweeteners (especially aspartame). Maintain stable blood sugar by eating every 3–4 hours. Staying hydrated (8–10 glasses of water daily) is equally important and is one of the most effective headache prevention strategies. Proper nutrition supports overall brain function and reduces the risk of headache triggers related to diet.
Conclusion
Headaches can be frustrating, but quick relief is possible with simple steps like staying hydrated, resting, using compresses, and choosing the right remedies or medications when needed. Understanding the type and cause of your headache plays a key role in finding the most effective solution.
More importantly, prevention and awareness are essential for long-term relief. By identifying triggers, maintaining healthy habits, and making small lifestyle adjustments, you can reduce how often headaches occur and manage them more effectively in the future.
Frequently Asked Questions
How can I get rid of a headache in 5 minutes?
You can try applying a cold pack to your forehead, gently massaging your temples and neck, and drinking water for quick relief. Acupressure on the area between your thumb and index finger can also help reduce pain fast.
How do I know if my headache is serious?
Seek immediate emergency care if your headache: came on suddenly and severely (thunderclap), is accompanied by fever, stiff neck, confusion, or vision changes, follows a head injury, or is the worst of your life. Seek prompt (same-day) care if headaches are progressive, worsening over days/weeks, or associated with one-sided weakness or speech difficulty.
How to know if a headache is a tumor?
While most headaches are not caused by tumors, brain-tumor-related headaches typically worsen progressively over weeks or months, are often worse in the morning or with position changes, and are accompanied by other neurological symptoms such as vision changes, weakness, seizures, or personality changes. If you experience these combined symptoms, consult a doctor promptly. Note: Isolated headaches without other symptoms are very rarely caused by tumors.
Can stress cause headaches?
Yes, stress is one of the most common causes of headaches, especially tension headaches. It can tighten muscles in your head and neck, leading to constant pressure and pain.
Can screen time cause headaches?
Yes, excessive screen time can strain your eyes and trigger headaches. Long hours on digital devices without breaks can worsen discomfort and fatigue.
Is it safe to take painkillers daily for headaches?
No. Taking OTC pain relievers more than 10–15 days per month can cause medication overuse headache (MOH), a chronic cycle where the medication itself causes daily headaches. If you find yourself taking painkillers this frequently, consult a doctor about preventive treatment options instead.